Patients with Aortic Stenosis can be treated with Transcatheter Aortic Valve Replacement (TAVI), a less invasive surgical procedure for Aortic Stenosis than traditional Aortic Valve replacement.
This procedure is often reserved for elderly, multi-morbid patients with high peri-operative mortality risk. This population represent a unique group, as they are usually extremely limited in their ability to perform physical activity prior to an intervention, may be limited by medications and are often severely deconditioned due to other co-morbidities.
Despite this, there is limited evidence of the effects of physical rehabilitation after TAVI. Through the Active Hospital pilot we aimed to assess the effects of exercise intervention on health-related quality of life and the physical functioning of patients receiving the TAVI procedure.
TAVI Pathway Overview
Pathway
Outpatient Appointment
Admission and surgery
Phone follow up
Outpatient follow up
Direct
Review of achievements and goals
Support and confidence building
Indirect
Governance framework
Culture Change
Resources
Interventions
Interventions were designed following consultation and engagement with patients and healthcare professionals within the TAVI procedure pathway. We mapped the existing pathway and designed interventions informed by the theoretical domains framework and COM-B model.
Motivational Interview (More minutes conversation)
During their admission our Physical Activity Champion conducted motivational interviews (that followed the structure of a More minutes conversation) with patients, who were identified if they had a stable Early Warning Score and were not on an end of life pathway.
Our Physical Activity Champion was trained in motivational interview techniques by the central Active Hospital team, as well as completing the online Active Conversations course to consolidate learning further.
A Patient Workbook was used during motivational interviews to give consistent structure to the conversation, help patients set their ambitions and plan how to achieve their goals.
Exercise program leaflets (Standing, Chair and Bed-based) were available for patients depending on their functional level.
All Active conversations were documented in the patient’s Electronic Patient Record.
A patient workbook was issued to patients before their first outpatient appointment, and this was revisited and used during the inpatient conversation with the Physical Activity Champion to give consistent structure to the conversation and to help the patient consider setting personal goals and plans.
The booklets were designed with behaviour change theories underpinning the content. Patient set goals can be a way to help patients keep focused and feel motivated. Consideration was given to both short and long term goals to help the change feel more achievable.
Achievements were reviewed at follow up phone calls and outpatient attendance.
Standing, Chair and Bed-based exercise programs were developed to support patients through their behaviour change.
The exercise booklets are designed to encourage ‘something rather than nothing’, as recommended by public health guidelines and The Royal Osteoporosis Society. They are not designed to bring about a training effect rather to support patients and their carers and families with some appropriate, easy-to-follow exercises to practice whilst in hospital and at home.
There is a focus on anti-gravity muscles in the lower limb, as these muscle groups are at particular risk of atrophy following a period of immobilisation, as well as some gentle aerobic work and upper limb strength. Exercises that cause strong trunk flexion are avoided for the older work group.
They were designed to require little or no equipment and are transferable to the home environment. The exercises were developed to ensure that all patients regardless of level of frailty or functional impairment could participate.
Pedometers and step counting
Pedometers and Step-Counting booklets were available for patients to support their behaviour change.
The use of wearables to monitor step counts is safe and acceptable to patients, and there is evidence that suggests that this can be an effective and cost effective intervention to assist behaviour change (1).
Reference:
Hobbs N, Godfrey A, Lara J, Errington L, Meyer TD, Rochester L, et al. Are behavioral interventions effective in increasing physical activity at 12 to 36 months in adults aged 55 to 70 years? A systematic review and meta-analysis. BMC Med. 2013;11:75
Patients undergoing the TAVI procedure are often elderly, multi-morbid patients with high peri-operative mortality risk. For all clinical pathways, but particularly those where patients have high mortality rates, a detailed review of potential side effects and poor outcomes is important to convince stakeholders of appropriate preparation. Integration into governance system is essential for patient safety. We conducted a systematic review of the literature around TAVI and exercise interventions, including mortality data before commencing the pathway interventions (pending publication).
High level and senior support for development and integration of interventions within the patient journey is critical to building change within the hospital environment. We liaised closely with senior figures throughout the design, delivery and maintenance phases of this pathway. We maintained a presence on the departmental governance meetings to ensure full integration of interventions within a robust governance framework.
Feedback from staff before training highlighted that one of the barriers to supporting and advising physical activity to patients was a lack of knowledge of what was available locally to which they could refer. A community navigator role was developed for the Active Hospital pilot across all our clinical pathways, providing one-to-one consultations with patients as well as providing advice and guidance to staff on where to find support for patients in the community. Their role was critical to ensure continuity of care through hospital admission to discharge to community environment.
An online map was developed to allow all staff and patients access to the wide range of community based classes and support throughout the region.

Physical Activity Champion
Our Physical Activity Champion was employed for one day per week to work on the TAVI pathway. The clinical champion was critical to the success of the project, and when recruiting we were looking for an enthusiastic, innovative and experienced professional with outstanding leadership and interpersonal skills.
The role included opportunities to develop clinical skills in behavioural change counselling and exercise medicine as well as develop managerial skills such as education, systems review and leadership.
As well as Trust induction, our Physical Activity Champion was given an induction to the Active Hospital project. – we developed an Active Hospitals Staff Induction document to help them with the induction process. They received training in motivational interview techniques from the central active hospital team, as well as completing the online Active Conversations course to consolidate learning further.
All Physical Activity Champions were supported through regular appraisal, using our Clinical Supervisor Meeting template and Personal Development Plan template.
Physical Activity Calculator
The Physical Activity Calculator is a modified version of the exercise vital sign (1, 2, 3) that was designed and incorporated into the Trust’s electronic record system. This validated self-reported tool was chosen it was felt practical and realistic for staff to deliver.
Physical activity levels are assessed and coded into three categories with a very brief advice prompt given depending on patient’s physical activity levels. The three categories are:
(1) Green (more than 150 minutes/week)
(2) Amber (30-150 minutes/week)
(3) Red (less than 30 minutes/week).
Brief advice, in the form of a 1 minute conversation, is given depending on physical activity levels.

References:
- Sallis R, Franklin B, Joy L, et al. Strategies for promoting physical activity in clinical practice. Prog Cardiovasc Dis 2015;57:375–86.
2. Coleman, K.J., et al., Initial validation of an exercise “vital sign” in electronic medical records. Med Sci Sports Exerc, 2012. 44(11): p. 2071-6
3. Department of Health and Social Care: UK CMO Physical Activity guidelines for older adults. Accessible from https://www.gov.uk/government/publications/uk-physical-activity-guidelines
Outcomes
Active Hospitals Pilot Oxford: Empowering patients to increase physical activity levels after Transcatheter Aortic Valve Implantation (TAVI)
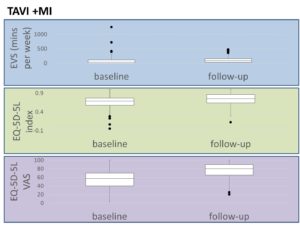
Over a 8-month period, 102 patients underwent TAVI and completed a baseline questionnaire. Of these, 89 (87%, age range 46 to 94 years) received an Active Conversation (Motivational Interview [MI]). In those that had TAVI + MI the median EVS at baseline was 30 minutes (interquartile range (IQR) 0.0, 120) increasing to 90 minutes (30, 150) at follow-up. Baseline median EQ-5D-5L index 0.69 (0.574, 0.763), and EQ-5D-5L visual analogue score (VAS) 57.5 (40, 70) increased to 0.751 (0.637, 0.867) and 80 (65, 90) respectively.
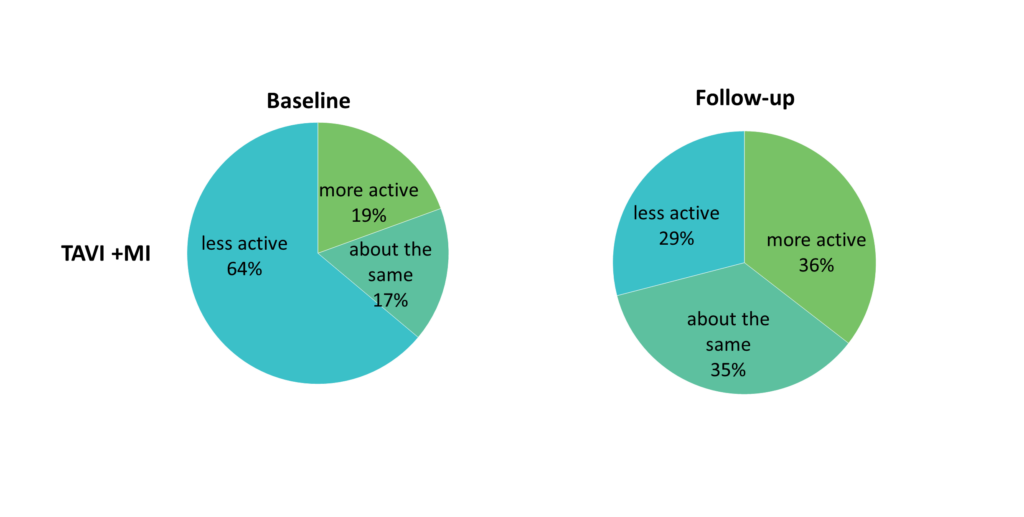
In those who had TAVI + MI, at baseline, 46 (64%) patients reported they were currently less active than their peers, with 12 (17%) about the same and 14 (19%) more active. At follow-up, 9 (29%) reported they were currently less active than their peers , 11 (35%) about the same and 11 (35%) more active.
Tips
Click on the numbers below for some tips from our Active Hospital team
1
For all clinical pathways, but particularly those where patients have high mortality rates, a detailed literature review of potential side effects and poor outcomes is important to convince stakeholders of appropriate preparation. Integration into governance system is essential for patient safety.
2
During our design phase we spoke with patients and relatives in clinic and on the ward. We learnt about their priorities and concerns and found that family members were playing a more significant role then we anticipated, which helped shape our interventions.
3
Be aware of what else is going on
It is important to be aware of other research and innovation programmes taking place at the same time. During our design phase, we learnt that the cardiology department was collaborating with a major program of work with NHS England and this led to some uncertainty and delays. Meeting with key stakeholders early helped facilitate the successful planning and delivery of both projects whilst minimising conflicts.
4
Design pathways with outcomes in mind
It is important to consider what outcome measures you are going to collect early in the design phase. Building data collection into the pathway will save time later in the process and is important for securing long term funding.
Despite a well designed mechanism for collecting data within this pathway, there were still barriers to overcome such as time pressures on staff and resources. We have designed a data collection tool to help you.
Build data collection, audit and quality improvement projects into your governance framework to sustain this in the long term.
Resources
Standing exercise programme
Chair based exercise programme
Bed based exercise programme